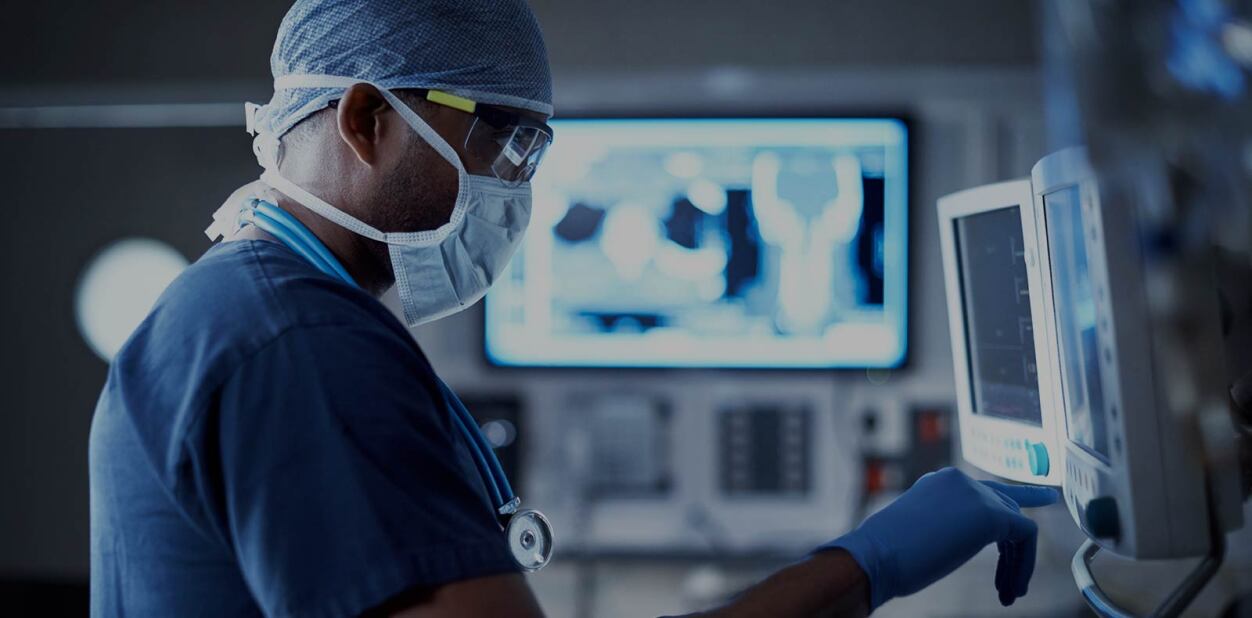
Hospitals have steadily increased their reliance on point-of-care testing (PoCT) devices to help manage patient care. This is certainly understandable; every healthcare organization is (or ought to be) focused on delivering the right care, at the right time, to increase quality and reduce costs. Gathering timely information about patients as close to the bedside as possible dramatically increases efficiency and enables rapid responsiveness, with measurable improvements in the quality of care delivered.
These improvements depend on ensuring the information produced by PoCT devices makes its way into the medical record as quickly and efficiently as possible. And not just any information, but the right information. Optimally, PoCT devices should be interfaced correctly to the enterprise so that data can be transmitted electronically, enhancing the accuracy and the timeliness of reporting.
The lack of a standard for HL-7 or POCT1-A messaging – a problem across virtually all of the healthcare IT industry – is particularly acute in PoCT, where some device manufacturers provide little or no interface support at all.
In addition, the competing priorities within the enterprise often mean that PoCT interfaces are not at the top of the list of IT projects. Whether the project is being done internally by IT staff, or through an outside interface services provider, there is typically a lot of pressure to complete the project as quickly as possible. This often leads organizations to stick to the basics, which is unfortunate.
The promised efficiencies of using PoCT devices cannot be fully realized without a methodical approach across the organization that addresses not just the technical requirements of proper installation, maintenance and operation, but also the people and process issues that will inevitably make the difference between more convenient patient care and actually improving the quality of care patients receive.
But it’s not just about efficiency; the organization’s regulatory obligations require these issues to be properly addressed as well.
PoCT is a laboratory function subject to CLIA requirements, and the ongoing oversight and accreditation required under HCVA. As such, PoCT in the hospital is subject to inspection and accreditation by the College of American Pathologists (CAP), and by the Joint Commission on Accreditation of Health Care Organizations (JCAHO). A formal training program for (and annual certification of) staff with respect to the proper operation of PoCT devices, together with ongoing evaluation of compliance, procedures for delivering feedback, and providing for retraining as needed, are among the many requirements.
Responsibility for ensuring that the organization meets its obligations is delegated to a PoCT manager, often a member of the lab staff. The need to develop, implement, and document compliance with these sorts of requirements, while standard operating procedure within the laboratory operation, presents unique challenges in the PoCT context.
In contrast with most other core lab functions that are handled by trained laboratory professionals, the operation of PoCT devices is usually the responsibility of the caregivers closest to the patient. While nursing staff are highly trained within their discipline, they are not usually knowledgeable about laboratory best practice. They also are not likely to be subject to direct management by laboratory personnel. And, while the use of PoCT devices is important to the delivery of care, it is one among many nursing staff responsibilities.
These challenges can make it difficult for a PoCT manager to get the job done, particularly when it comes to monitoring staff compliance. So how can PoCT managers successfully manage thousands with no direct management chain of command?
The answer to all of this lies in intelligent system design that considers the PoCT manager’s need for additional information and feedback. The system can be engineered to provide feedback from the instruments that can help in ensuring proper procedure is being followed.
PoCT systems represent a rich source of data, yet most of the data management tools available do not take full advantage of the full breadth of data to support PoCT management in achieving its goals.
Beyond managing the connectivity and getting the results into the EMR, the PoCT data can actually drive quality improvements in how care is delivered.
And that’s the point of point-of-care testing.
Analyzing incoming data when something of potential concern is identified enables teachable moments that are vital to improving care. Let’s say, for example, that a PoCT manager gets a message from a device that three tests were performed on the same patient within moments of each other. That message could then trigger a meeting to discuss the particular circumstances. If protocol says one finger stick, why are there three? Armed with this information, lab professionals can take the right action.
This type of critical intervention is enabled only by advances in technology and process. Technology enables the accountability process, and that can drive marked improvements in overall performance. And that’s a goal everyone can agree upon.
About the Author
Hugh Badian is founder and CEO of Logical Connections, a leading healthcare software solutions company. Logical Connections is a healthcare IT solutions provider with strong roots in the clinical and anatomic pathology laboratory.