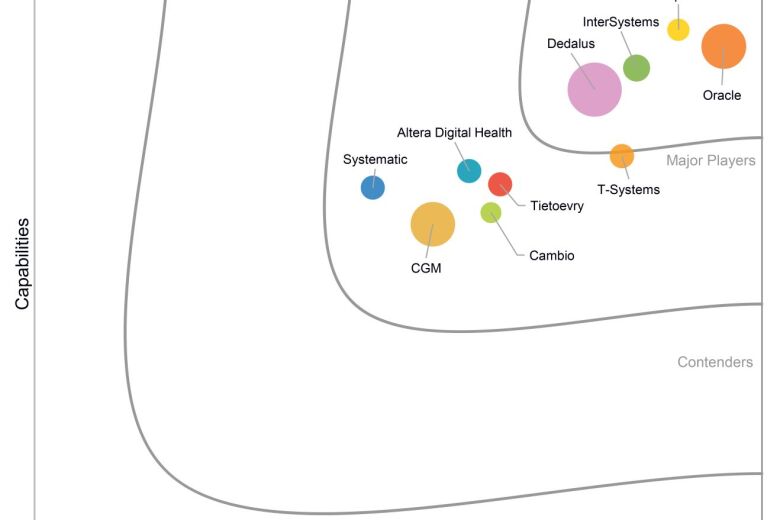
The TrakCare Operating Theatres (OT) module, seamlessly connects every point within the OT department into the familiar single, unified patient record. The same digital record used across wards, outpatients, emergency department, diagnostics and management, TrakCare OT enables safer surgery, smoother handovers and better use of scarce theatre capacity.
Real-time updates keep your entire clinical and operational team in the loop, while everything is tracked on a single, continuous patient record.
Delivering what matter to clinical teams every day - from preventing delays and bottlenecks to improving handovers and reducing variation in care. Fewer delays, fewer handover failures, and clearer decision-making before, during and after surgery.
TrakCare Operating Theatres is not about replacing one theatre system with another.
It is about placing theatres where they belong: at the centre of a connected, reliable and resilient patient record — supporting safer care, better flow and sustainable performance.
Benefits

Impact for the Health Boards
- Fewer delays and cancellations caused by missing or conflicting information
- Safer surgical pathways through reliable, real-time data
- Improved flow across theatres, wards and critical care
- Stronger data quality for performance management and improvement
Improving patient flow and reducing waiting lists
Reducing elective backlog depends on more than theatre scheduling alone. It requires alignment between theatres, beds, diagnostics, staffing and post-operative capacity.
TrakCare enables this by:
- Making theatre activity visible to bed management and site teams in real time
- Allowing constraints such as bed capacity or outbreaks to be seen early by theatre teams
- Supporting faster turnaround through clearer coordination across departments
Potential Impact for the NHS:
- More procedures completed per session
- Fewer late starts and early finishes
- Better delivery against elective recovery targets
Potential Impact for the NHS:
- More procedures completed per session

Potential Impact for the NHS:
- More procedures completed per session
Enabling the shift to prevent harm rather than creating it
Safer surgery starts well before the patient enters theatre.
By connecting pre-assessment, diagnostics and historical clinical data directly into the theatre workflow, TrakCare helps teams identify and mitigate risk earlier — reducing last-minute cancellations and post-operative complications.
This supports:
- Earlier identification of comorbidity-related risk
- Better alignment of antibiotic prophylaxis with allergies and microbiology
- Reliable capture of data for audit, quality improvement and surveillance
Potential Impact for the NHS:
- Fewer avoidable cancellations
- Reduced complications and length of stay
- Stronger insight into surgical outcomes and variation
Challenges —
and how TrakCare addresses them
Challenge | Solution |
| Multiple systems in theatres | A single EPR with one login and one patient record |
| Siloed information across departments | Real-time, shared data across theatres, wards, ICU, pharmacy and diagnostics |
| Fragile handovers to recovery and critical care | Structured data flowing with the patient, not stopping at the theatre door |
| Operational blind spots | Hospital-wide visibility of theatre activity and downstream capacity |
Frequently Asked Questions
TrakCare Operating Theatres embeds theatre workflows into the enterprise patient record, so documentation, timings and safety steps are visible across wards, recovery, ICU, ED and clinics. This reduces duplication, improves coordination and strengthens governance.
- Immediate availability of operative and anaesthetic notes
- Reduced information loss at handover
- Fewer transcription errors
- Clear audit trails
- Consistent completion of safety checklists
By improving visibility of list progress and reducing system switching, TrakCare supports smoother coordination. Early optimisation and effective training help ensure workflows remain efficient.
Recovery, wards, ICU and emergency teams can see the plan without waiting for scanning, transcription or chasing theatres.
Digitisation improves traceability and audit, but it does not replace the shared team conversation during sign-in, time-out and sign-out.
- Late starts
- Turnaround times
- Cancellation reasons
- Downstream bed constraints
How that data is used is determined by local governance and leadership. A mature approach focuses on system constraints and service improvement rather than simplistic individual attribution.
It will not remove cancellations driven by clinical deterioration, emergency pressures or workforce shortages.
Clinical care continues using agreed contingency processes, with retrospective documentation entered once systems are restored. Safe care delivery takes priority.
- Create staff rosters
- Manage workforce contracts or on-call rotas
- Decide staffing levels
- Automatically prioritise cases
- Replace procurement or stock control systems
- Make clinical decisions