
By Jonathan Teich, MD, PhD, CMIO, Director of Product Management, HealthShare
Since COVID-19 began roaring through communities around the world early this year, healthcare leaders have adapted their approach for each phase of the pandemic, and information systems have played an essential part. In the early phase, when cases were mainly travelers from a few countries, healthcare organizations implemented screening processes in triage systems to detect potentially infected patients. Then came the great surge of infections in the spring; one vital step in the campaign to flatten the curve and avoid overwhelming health system capacity was the development of acute-care dashboards that analyzed metrics such as hospital admissions, ventilator usage, and patient characteristics. Had we not used these insights to inform closures and social-distancing policies, evidence suggests the U.S. alone might have had 10 to 20 times more COVID-19 cases.
Now, most countries are beginning to eliminate lockdowns and reopen businesses, changing policies that were good for infection prevention but bad for a society intent on functioning. But the challenge is to do both. To maintain control over the next year, we must adapt once more and find a solution to the newest challenge: how can public health systems keep the pandemic suppressed and prevent new outbreaks as people return to their lives?
A large part of the answer is a combination of extensive testing, contact tracing, and syndromic surveillance. These allow healthcare leaders to identify “hotspots” where new cases are sprouting and stamp them out before they spread out of control. With syndromic surveillance, healthcare organizations can monitor trends and pinpoint unusual variations in a community: a spike in hospital admissions, medical visits and phone calls for coughs and fevers, or abnormal lab tests. Displays and alerts about such events can help public health agencies identify troubling changes in a given neighborhood; they can then concentrate scarce resources such as contact tracers, medical staff, or supplies where they are needed most. Syndromic surveillance can actually be used for all sorts of large-scale health concerns, from COVID-19 to toxic spills to outbreaks of gastrointestinal illness.
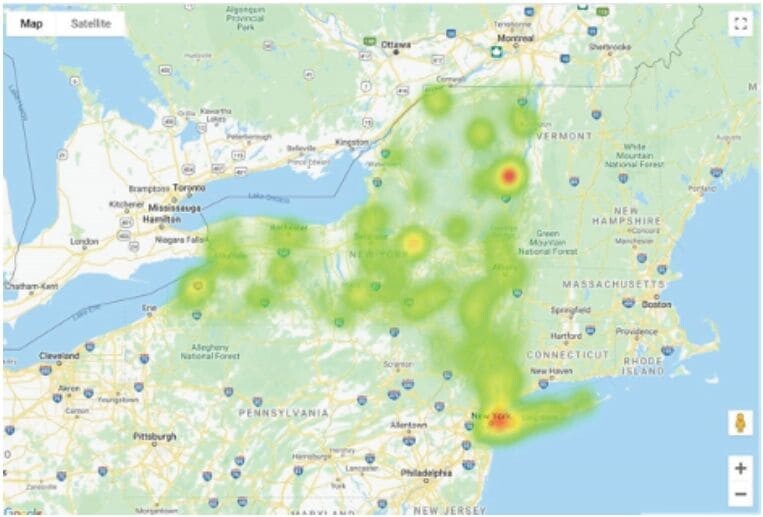
The execution of any successful syndromic surveillance program, however, has a few key requirements: a need for plenty of clean data, and the power of high capacity and throughput to continually process that data in near-real time. Several InterSystems customers have created COVID-19 dashboards for the acute phase; they’re now starting to conduct syndromic surveillance through HealthShare using the Unified Care Record and Health Insight. By aggregating high-volume data from numerous health systems and medical practices, HealthShare helps customers assemble the information they need to understand what’s going on in their cities and towns. Customers can capture data on COVID-19 testing, other labs and vital signs, chief complaints and diagnoses, comorbidities, medications, use of ICU beds, and more. They can produce maps and charts using the Health Insight interface or third-party visualization tools. They can provide infographics for the community, reports for state and national agencies, information for gauging need for additional personal protective equipment (PPE) or testing supplies. Using syndromic surveillance techniques, they can detect when a key parameter jumps above a certain threshold, and notify public health officials of the emerging hotspot, early enough to help guide movement of supplies and resources. The early heads-up that HealthShare aggregated and normalized information provides is a critical advantage in the fight against the pandemic.
InterSystems development teams are hard at work developing additional advanced tools and displays, while clinical informatics staff are curating content such as emerging codes for the new COVID-19 PCR and antibody tests, comorbidity diagnostic codes and value sets, risk factor parameters as new evidence comes out, and updated query templates to produce the most useful reports possible to guide action. HealthShare customers can make use of these to help make analytic queries reflecting your own data.
COVID-19 is a very extensive and serious public health crisis, but it is not the first and will not be the last. After Hurricane Katrina, health information exchange helped displaced refugees access their medications; in the 2014 Ebola crisis, contact tracing information was vital to containing the spread. From epidemics to earthquakes to hurricanes and more, rich sharing and use of data is necessary to minimize the impact of health disasters. InterSystems is proud to support you, our customers, as you play vital roles in addressing regional, national, and worldwide health crises.
This story originally appeared the July 10, 2020 - HealthShare Connections News Flash No.3: COVID-19 Pandemic newsletter



























